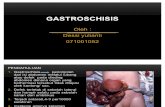
Omphalocele vs gastroschisis
-
Upload
c-lah-divere -
Category
Health & Medicine
-
view
744 -
download
3
Transcript of Omphalocele vs gastroschisis

ABDOMINAL WALL DEFECTSOMPHALOCELE VS GASTROSCHISIS
Rusila TikoitogaMBBS 42016

OBJECTIVES• Background• Epidemiology• Etiology• Pathophysiology• Clinical Features• Diagnosis• Management• Prognosis

History
• 1634 - Ambroise Paré (French barber surgeon) first described Omphalocele.
• Derived from Latin word “Omphalos” meaning prominence or navel.
• 1733 – James Calder (Scottish neonatal surgeon) first described Gastroschisis.
• Derived from the Greek word “Gaster”(Gastro) meaning belly and “schisis” meaning to tear or split from "

Epidemiology Gastroschisis Incidence - 4 per 10,000 M:F is 1:1• 10-15% association with
congenital anomalies such as CHD(VSD), cleft palate and intestinal atresia
• 40% are premature/SGA
Omphalocele Incidence - 3 per 5,000 M:F is 1.5:1 >70% association with
congenital anomalies such Bowel atresia, Imperforated anus, Trisomies 13, 18, 21, Beckwith-Wiedemann Syndrome & Pentalogy of Cantrell

Etiology• Gastroschisiso Congenital abdominal wall defect towards the
right side of the umbilicus and protruded bowel is not covered by a membrane.
o Failure of migration and fusion of the lateral folds of the embryonic disc on the 3rd-4th week of gestation.
o Disruption of the right omphalomesenteric artery as midgut returns to abdomen by the 10th week causing ischemia of the abdominal wall and weakness then herniation.
o Rupture of omphalocele
• Omphaloceleo Congenital abdominal wall defect
with protrusion of abdominal viscera contained within a parietal peritoneum and amniotic membranous sac with Wharton’s jelly.
o Due to failure of the midgut to return to abdomen by the 10th week of gestation during midgut rotation.

Risk FactorsOmphalocele
• Increased maternal age• Twins • High gravida• Consecutive children
Gastroschisis• Young maternal age • Low gravida• Prematurity• Low birth-weight
secondary to IUGR

OMPHALOCELE GASTROSCHISIS

OMPHALOCELE GASTROSCHISIS

Embryology of GIT


Clinical Features
OMPHALOCELE
• central defect of the abdominal wall beneath the
umbilical ring.
• Defect may be 2-12 cm (Small-<5cm)(Large>8cm)
• Always covered by sac
• Sac is made of amnion, Wharton’s jelly and
peritoneum
• The umbilical cord inserts directly into the sac in an
apical or lateral position.
• Small contains intestinal loops only. Large may
involve liver, spleen and bladder, testes/ovary
• >50% have associated anomalies
GASTROSCHISIS• Defect to the right of an intact umbilical cord allowing
extrusion of abdominal content
• Umbilical cord arises from normal place in abdominal
wall
• Opening <=5 cm
• No covering sac (never has a sac )
• Evisceration usually only contains intestinal loops
• Bowels often thickened, matted and edematous
• 10-15% have associated anomalies
• 40% are premature/SGA

Diagnosis• Alpha-feto-protein-synthesized in fetal liver and
excreted by fetal kidneys and crosses placenta by 12 weeks.
• Elevated maternal AFP - neural tube defects, abdominal wall defects, duodenal or esophageal atresia
• 40% false positive rate• Fetal ultrasound after 14 weeks gestation is the
confirmatory test.

Prenatal Ultrasound
• Normal umbilical cord insertion site
• Small bowel loops seen in the amniotic cavity
• No covering membrane over the loops of bowel
• Can include stomach and large bowel
• Majority occur to the right of the umbilical cord
Gastroschisis

Prenatal Ultrasound
• Umbilical cord insertion is typically midline on the mass
• Located centrally• Contents are intestinal
loops and maybe liver, spleen and gonads.
Omphalocele

ManagementPerinatal Management• Maternal Screening Fetal Ultrasound = positive findings Alpha-feto-protein elevated = 90%
Omphalocele 10% Gastroschisis• Prenatal counselling

Pre-operative Management• ABC• Heat Management
– Sterile wrap or sterile bowel bag– Radiant warmer
• Fluid Management– IV bolus 20 ml/kg LR/NS– D10¼NS 2-3 maintenance rate
• Nutrition– TPN (central venous line )
• Abdominal Distention– OG/NG tube– urinary catheter
• Infection ControlBroad-spectrum antibiotics - Ampicillin and Gentamycin
• Closure of the Defect

Omphalocele • Conservative
1. Large omphalocele (10-12cm) apply topical application - Betadine ointment or silver sulfadiazine to the intact sac.
2. Secondary eschar formation and granulation.
3. Healing lasts for 12 months then repaired as ventral hernia.
o Primary Closure Small defects (<4cm) excision of the sac and
closure of the fascia and skin over the abdominal contents
o Mesh patch Medium defects (6-8cm)

• Post operative careo NICUo Ventilationo Feeding:
– Minimal volumeo 48 hrs Antibioticso Hernia dealt with at 1
yr old

Gastroschisis• Primary closure
o If bowel easily reduced• Staged closure
o Silo fashioning:Sac excisedSilo sewn to rectus fascia/full thickness

• Post operative careo NICUo Feeding delayed for weekso Oral stimulation/sucking
reflexo Broad spectrum
antibiotics

Long Term OutcomesOmphalocele• Small - recover well• Large:
– Gastro-oesophageal reflux - 43%– Majority improve over time– 20% pulmonary insufficiency– Respiratory Infections– Asthma– Feeding difficulties;
• 60% with giant omphalocele• May need gastrostomy for feeding
– Failure to thrive
Gastroschisis• Generally excellent if no atresia• NEC:
– 18.5% of neonates more with formula– Bowel loss - short gut syndrome
• Cryptorchidism:– 15-30%– Due either being outside/prematurity– Replacement and orchidopexy by 1 yr
• 60% have psychosocial stress if umbilicus sacrificed

Summary

References:• Up to Date• Medscape• O.P Ghai E.pediatrics• Rudolph’s pediatrics